What Is Spondylolisthesis?
Spondylolisthesis describes the forward displacement of a vertebra in relation to the vertebra below. The term “spondylolisthesis” was coined in 1854, from the Greek “vertebra” and “slipperiness”. It can be a sign of spinal instability and patients can have back or leg symptoms. These “slips” occur most commonly in the lumbar spine.
Spondylolisthesis is officially categorized into five types:
- Dysplastic spondylolisthesis is a true congenital slippage of the vertebra that occurs because of abnormal formation of the spine. It is very rare, but when seen it tends to progress rapidly and is often associated with severe neurological problems.
- Isthmic spondylolisthesis is the most common form of spondylolisthesis seen in 5-7% of the U.S. population. It is caused by a bony defect or fracture in the pars interarticularis, an area located on the lamina (roof) of the vertebrae.
- Degenerative spondylolisthesis is the result of aging and wear and tear in the spine. Degenerative spondylolisthesis with spinal stenosis (narrowing) is one of the most common indications for spine surgery among older adults.
- Traumatic spondylolisthesis is very rare and may be associated with acute fracture of the spine.
- Pathologic spondylolisthesis is also very rare. This type can occur following damage to the spine from metastases (spinal tumor) or metabolic bone disease, such as osteoporosis.
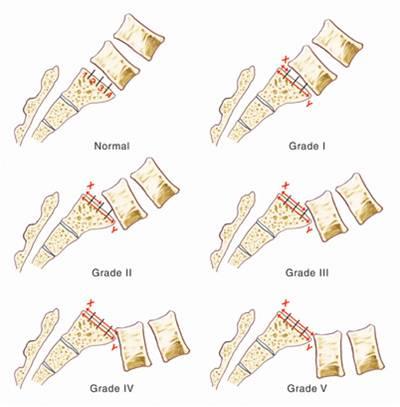
The most common grading system for spondylolisthesis is the Meyerding grading system. The system categorizes severity based upon measurements on the x-ray to describe how far forward the vertebra has slipped.
- Grade 1 is 0-25%
- Grade 2 is 25-50%
- Grade 3 is 50-75%
- Grade 4 is 75-100%
- Over 100% is spondyloptosis, when the vertebra completely falls off the supporting vertebra
Signs and Symptoms
Spondylolisthesis, especially the degenerative type, and spinal stenosis typically causes lower back pain, muscular spasm, and/or pain with radiation to the buttocks or legs. It may cause leg weakness or numbness.
Non-surgical Treatment
Treatment is based on the characteristics of the patient’s symptoms. Acute symptoms may sometimes be relieved with 1-2 days of bed rest and activity restriction. In addition, medications such as anti-inflammatories or muscle relaxants can alleviate some symptoms. Braces have a minor role, but it can be worn for comfort as needed for a short period of time. Physical therapy is often prescribed to increase back conditioning. Muscle strengthening can help reduce the frequency and intensity of the spasms. Epidural steroid injections may be helpful as well.
Surgical Treatment
Dr. Cho recommends surgery:
- If non-surgical treatments do not relieve back and leg pain.
- If the slip is progressing (getting worse).
- If the slip is causing nerve damage.
- If the slip is Grade 3 or above.